
Medical disclaimer: This article is for informational purposes only and does not constitute medical advice. If you have type 2 diabetes or any other medical condition, always consult your physician or a licensed healthcare provider before starting or modifying any exercise or nutrition program. Individual circumstances vary, and your care team is the best source of guidance for your specific situation.
If you have type 2 diabetes, you've heard it a hundred times: you need to exercise more.
Your doctor has said it. The pamphlets say it. Every article you've read says it. And they're right — exercise is one of the most powerful tools available for managing blood glucose, improving insulin sensitivity, and protecting your cardiovascular health. The research is overwhelming and unambiguous.
But knowing you should exercise and actually doing it consistently are two entirely different problems. And for people managing type 2 diabetes, the consistency gap isn't just frustrating — it directly impacts health outcomes.
So the real question isn't whether exercise helps. It's: how do you build a routine you'll actually sustain, week after week, month after month?
That's where the science of gamification enters the picture — and where a landmark clinical trial offers genuinely encouraging answers.
What the Research Shows
In 2021, researchers published results from the iDiabetes trial in JAMA Network Open — one of the largest randomized controlled trials ever conducted on gamification and physical activity in people with type 2 diabetes.
The study enrolled 361 adults with type 2 diabetes. The average age was 52.5 years, approximately 56% were women, and roughly 51% were Black — making this one of the more diverse clinical populations studied in digital health research. Participants were randomized into three groups: a control group that received standard step tracking, a competition-based gamification group, and a support-based gamification group.
The results were striking:
- Competition-based gamification produced +606 additional steps per day compared to the control group (P=.003)
- Support-based gamification produced +503 additional steps per day compared to the control group (P=.01)
- The entire intervention was fully remote and automated, delivered through wearable devices — no in-person coaching required
To put those numbers in perspective: an extra 500 to 600 steps per day translates to roughly 20 to 25 additional minutes of walking. That's clinically meaningful. Research consistently shows that even modest increases in daily movement improve insulin sensitivity, support blood glucose regulation, and reduce cardiovascular risk factors.
What makes this study particularly powerful is that it wasn't conducted on college students or fitness enthusiasts. These were real adults managing a chronic condition, and the gamification intervention helped them move more — consistently — without requiring a gym membership, personal trainer, or massive lifestyle overhaul.
Why Consistency Matters More Than Intensity for Diabetes
There's a common misconception that exercise needs to be intense to be effective for blood glucose management. The research tells a different story.
The American Diabetes Association recommends at least 150 minutes per week of moderate-intensity physical activity — that's about 30 minutes a day, five days a week. Notice the emphasis: moderate intensity. Not high intensity. Not grueling. Not the kind of workout that leaves you on the floor.
Why does consistency matter so much? Because of how exercise affects insulin sensitivity:
- Exercise increases glucose uptake by muscles, which directly lowers blood sugar levels during and after activity
- Insulin sensitivity improves for 24 to 72 hours after exercise, meaning regular movement creates a sustained metabolic benefit
- Gaps longer than two consecutive days can reduce the insulin-sensitizing effects you've built up
- Cardiovascular health benefits compound over time, but only if the habit is maintained
This means that a person who walks briskly for 20 minutes every day is doing more for their blood glucose management than someone who does one intense gym session per week and sits the rest of the time. Frequency and regularity are the variables that matter most — a principle backed by decades of adherence research.
And that's exactly the problem — because showing up every day is the hardest part.
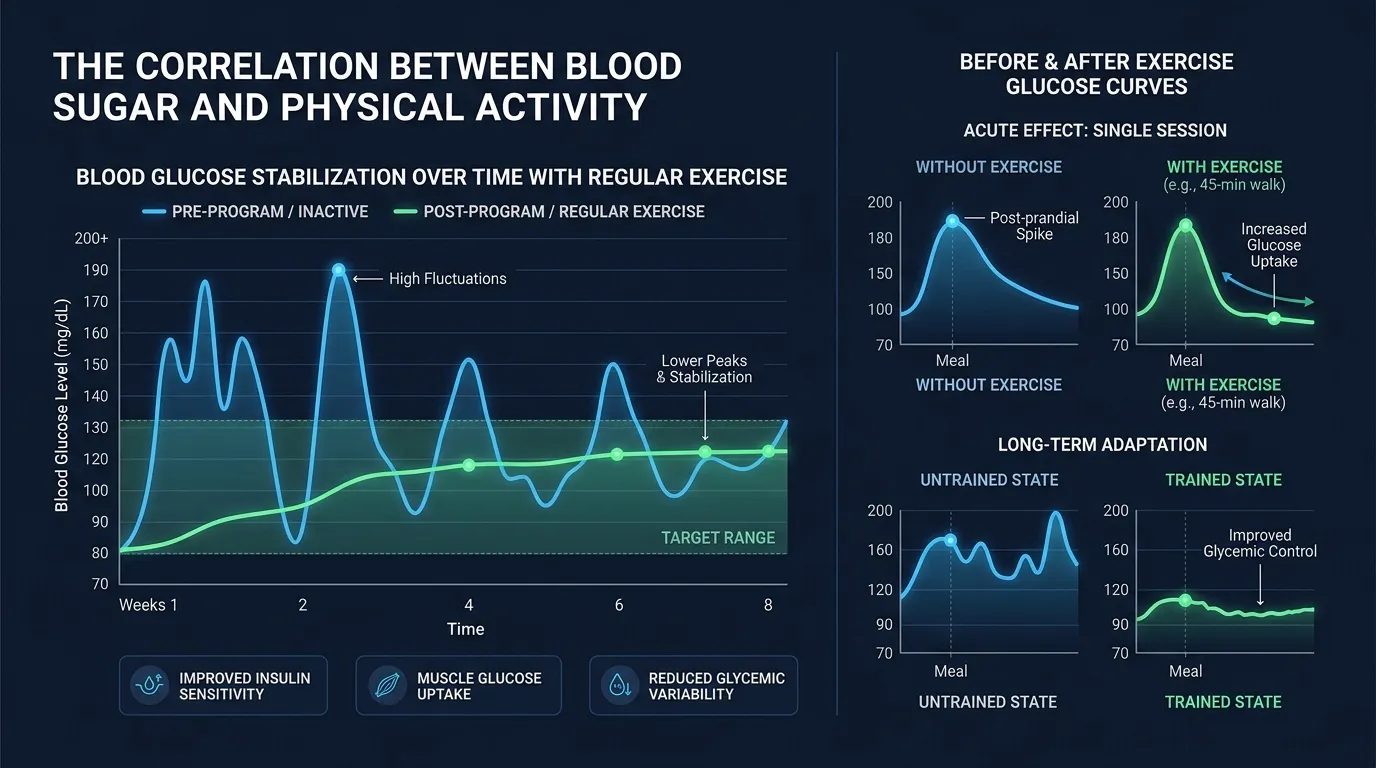
The Consistency Problem: Why People With Diabetes Struggle to Stay Active
If you have type 2 diabetes and you've struggled to maintain an exercise routine, you're not alone — and it's not a willpower failure. There are real, documented barriers that make consistency harder for people managing this condition:
- Fatigue and energy fluctuations. Blood sugar variability can make energy levels unpredictable. Some days you feel fine; other days the idea of a workout feels impossible.
- Exercise feels like another medical task. When your days already include monitoring blood glucose, managing medications, and watching your diet, adding exercise to the "medical to-do list" can feel overwhelming.
- Fear of blood sugar drops. Concerns about hypoglycemia during or after exercise can create anxiety that discourages activity.
- No immediate feedback loop. You can't feel your insulin sensitivity improving in real time. The benefits of today's walk are invisible — which makes it easy to skip.
- Programs designed for the general population. Most fitness apps don't account for the unique needs, concerns, and daily reality of someone managing a chronic condition.
These aren't excuses. They're legitimate obstacles — and they explain why telling someone with diabetes to "just exercise more" is about as helpful as telling someone with insomnia to "just sleep better." It's the same willpower myth that fails across all populations.
The question is: what actually works to overcome these barriers? The iDiabetes trial points to a clear answer.
How Gamification Solves the Consistency Problem
The iDiabetes trial didn't just show that gamification works — it showed why it works, by testing two distinct approaches.
Competition Mechanics (+606 Steps/Day)
The competition arm placed participants in small groups where they could see how their step counts compared to others. This isn't about being the fittest person in the room — it's about the psychological power of social comparison. When you can see that others like you are hitting their step goals, two things happen:
- Social norming: You see that regular activity is achievable, not exceptional. It shifts your perception of what's realistic.
- Gentle accountability: Knowing that your activity is visible to others creates just enough motivation to lace up your shoes on days when you'd otherwise skip.
Support Mechanics (+503 Steps/Day)
The support arm paired participants with teammates who could encourage each other. This taps into a different but equally powerful motivational system — the human need for connection and mutual accountability. When someone is counting on you, showing up feels less like a chore and more like keeping a promise.
Automated, Remote Delivery
Perhaps the most important finding: the entire gamification system was delivered remotely and automatically through wearable devices. No clinic visits. No in-person coaching sessions. No scheduling logistics. The participants received the behavioral nudges they needed through the technology they were already carrying.
This matters enormously for real-world application. A system that requires you to show up at a specific time and place adds friction. A system that meets you where you are — on your phone, on your wrist, in your daily life — removes it.
Build a routine that actually sticks
Take the free 2-minute assessment and get a personalized workout plan designed around your life, your fitness level, and the science of habit formation.
Take the Free Assessment Free · 2 minutes · No credit card
Blood Glucose, Nutrition, and Exercise Safety
Important: The information in this section is general and informational only. It is not medical advice and should not replace guidance from a licensed healthcare provider. Blood glucose management is highly individual, and incorrect approaches to nutrition and exercise can have serious health consequences — including potentially life-threatening situations. Always consult with a licensed healthcare specialist for personalized advice about managing blood sugar levels around exercise.
For people with type 2 diabetes, exercise doesn't happen in isolation — it interacts with what you eat, when you eat, and how your body processes glucose. Understanding the general relationship between blood glucose, food, and physical activity can help you approach exercise more safely, but the specifics will depend on your individual health profile.
Here are some general considerations that people with type 2 diabetes may want to discuss with their healthcare provider:
- Blood sugar can fluctuate during and after exercise. Physical activity generally affects blood glucose levels, but the direction and magnitude of that effect can vary depending on the type of exercise, its duration and intensity, your medications, and when you last ate. Your doctor or diabetes educator can help you understand what to expect and how to prepare.
- Timing of meals and snacks around exercise may matter. Some people find it helpful to plan when they eat in relation to when they exercise, but the right approach depends on your medication regimen, your typical blood sugar patterns, and your individual response to activity. Your healthcare team can provide personalized guidance.
- Hydration is important. Staying well-hydrated supports overall health and can influence how your body responds to exercise. Water is generally the best choice, but your provider can advise based on your specific needs.
- Monitoring is a valuable tool. Checking blood glucose before and after exercise — especially when you're starting a new routine — can help you and your healthcare provider understand how your body responds and make informed adjustments.
- Be prepared for unexpected changes. Having a plan for how to respond if your blood sugar goes too low or too high during exercise is an important safety measure. Your healthcare provider can help you create this plan.
The goal of this section is simply to highlight that nutrition and blood glucose management are important considerations for people with type 2 diabetes who exercise. This is not a substitute for professional medical advice. Every person's situation is different, and what works for one individual may not be appropriate — or may even be harmful — for another. Please consult with a licensed healthcare specialist who can assess your individual needs and provide personalized recommendations.
Getting Started Safely
Before diving into a new exercise routine, there are a few important steps to take — especially when managing type 2 diabetes:
- Talk to your healthcare provider. Discuss your plans, any medications that affect blood sugar during exercise, and what precautions to take. This is especially important if you're on insulin or sulfonylureas.
- Start gradual. You don't need to go from sedentary to 150 minutes per week overnight. Start with 10-minute walks after meals — a strategy that research shows is particularly effective for post-meal blood glucose management.
- Monitor your blood sugar. Check levels before and after exercise as you're building your routine, so you learn how your body responds to different types and durations of activity.
- Keep a fast-acting carbohydrate nearby. Glucose tablets, juice, or fruit can quickly address low blood sugar if needed during activity.
- Wear proper footwear. Foot health is especially important for people with diabetes. Invest in supportive, well-fitting shoes.
- Build up progressively. Add 5 to 10 minutes per week until you reach your target. Gradual progression reduces injury risk and builds confidence.
Medical disclaimer: Always consult your healthcare provider before starting a new exercise program, especially if you have type 2 diabetes or other medical conditions. This article is for educational purposes and does not constitute medical advice.
How FitCraft Applies This Research
The iDiabetes trial proved a principle: when you wrap exercise in the right behavioral framework, people with type 2 diabetes move more. FitCraft is built on that exact principle — and extends it.
- AI-personalized programming. FitCraft's AI coach adapts workouts to your fitness level, available equipment, and schedule. You take a 32-step diagnostic assessment, and the system builds a program specifically for you — designed by an Ivy League-trained exercise scientist, NSCA-certified strength coach. If you need to start with short, low-intensity sessions, that's exactly what you'll get.
- Competition mechanics that actually work. Just like the iDiabetes trial's competition arm (which produced +606 steps/day), FitCraft incorporates social comparison and competitive elements that create gentle, motivating accountability without making you feel like you're in a fitness boot camp.
- Self-chosen goals and progression. Autonomy matters. FitCraft lets you set goals that make sense for your life and then tracks your progression with streaks, quests, collectible cards, and leveling systems. You see your progress after every single session — not in 90 days when the scale finally moves.
- Streak-based accountability. The iDiabetes trial showed that consistent daily nudges drive results. FitCraft's streak system creates that same gentle pressure — not guilt-based, but reward-based. You show up because you don't want to break your streak, and that's a fundamentally different motivation than "my doctor told me to."
- Fully remote, on your schedule. Like the iDiabetes intervention, FitCraft is entirely app-based. No gym required. No scheduling conflicts. Workouts meet you where you are — at home, on the road, or wherever you have 15 minutes and a phone.
The research shows that the right system can help people with type 2 diabetes walk 500 to 600 more steps every day. FitCraft takes that research and builds a complete, personalized fitness experience around it — turning exercise from a medical obligation into a daily practice you genuinely look forward to.
Frequently Asked Questions
How much exercise do you need with type 2 diabetes?
The American Diabetes Association recommends at least 150 minutes per week of moderate-intensity physical activity for adults with type 2 diabetes. This can include brisk walking, cycling, swimming, or structured workouts. Even small increases in daily movement — such as an extra 500 to 600 steps per day — are clinically meaningful and can improve insulin sensitivity and blood glucose management.
Does gamification help people with diabetes exercise more?
Yes. The iDiabetes trial, a large randomized controlled trial published in JAMA Network Open (2021) with 361 adults with type 2 diabetes, found that competition-based gamification increased daily steps by 606 (P=.003) and support-based gamification increased daily steps by 503 (P=.01). The intervention was fully remote and delivered automatically through wearable devices, demonstrating that gamification can meaningfully increase physical activity in people with diabetes.
Is walking enough exercise for type 2 diabetes?
Walking is an excellent form of exercise for people with type 2 diabetes. Research consistently shows that regular walking improves insulin sensitivity, helps regulate blood glucose levels, and supports cardiovascular health. The key is consistency — walking regularly matters more than occasional intense workouts. Starting with daily walks and gradually increasing duration and pace is a safe, effective strategy.
What is the best fitness app for someone with type 2 diabetes?
Look for an app that prioritizes consistency over intensity, since regular moderate activity is what matters most for blood glucose management. FitCraft uses gamification — streaks, quests, competition mechanics, and progression systems — to help you build a daily exercise habit. Programs are designed by an Ivy League-trained exercise scientist, NSCA-certified strength coach and personalized by AI to match your fitness level, equipment, and schedule. Always consult your healthcare provider before starting a new program.
How do I stay consistent with exercise when I have diabetes?
Consistency is the biggest challenge — and it's where most people struggle. Research shows that gamification elements like streaks, social accountability, and competition can significantly increase daily physical activity. The iDiabetes trial found that gamified programs helped adults with type 2 diabetes walk over 500 additional steps per day compared to controls. The key is finding a system that makes showing up feel rewarding in the moment, rather than relying on willpower alone.