- A single workout transiently raises cortisol. The spike is small below about 60 percent of VO2max and steeper above it. Levels return to baseline within a few hours.
- Across 12 weeks of regular moderate training, baseline cortisol and stress reactivity tend to fall. Yoga and continuous aerobic exercise produce the largest reductions.
- Overtraining does not produce sky-high cortisol. It produces a blunted, flattened response. The fix is more recovery, not more discipline.
- The TikTok "cortisol face" trend is mostly a myth. True cortisol-driven puffiness shows up in Cushing's syndrome, not in everyday stress.
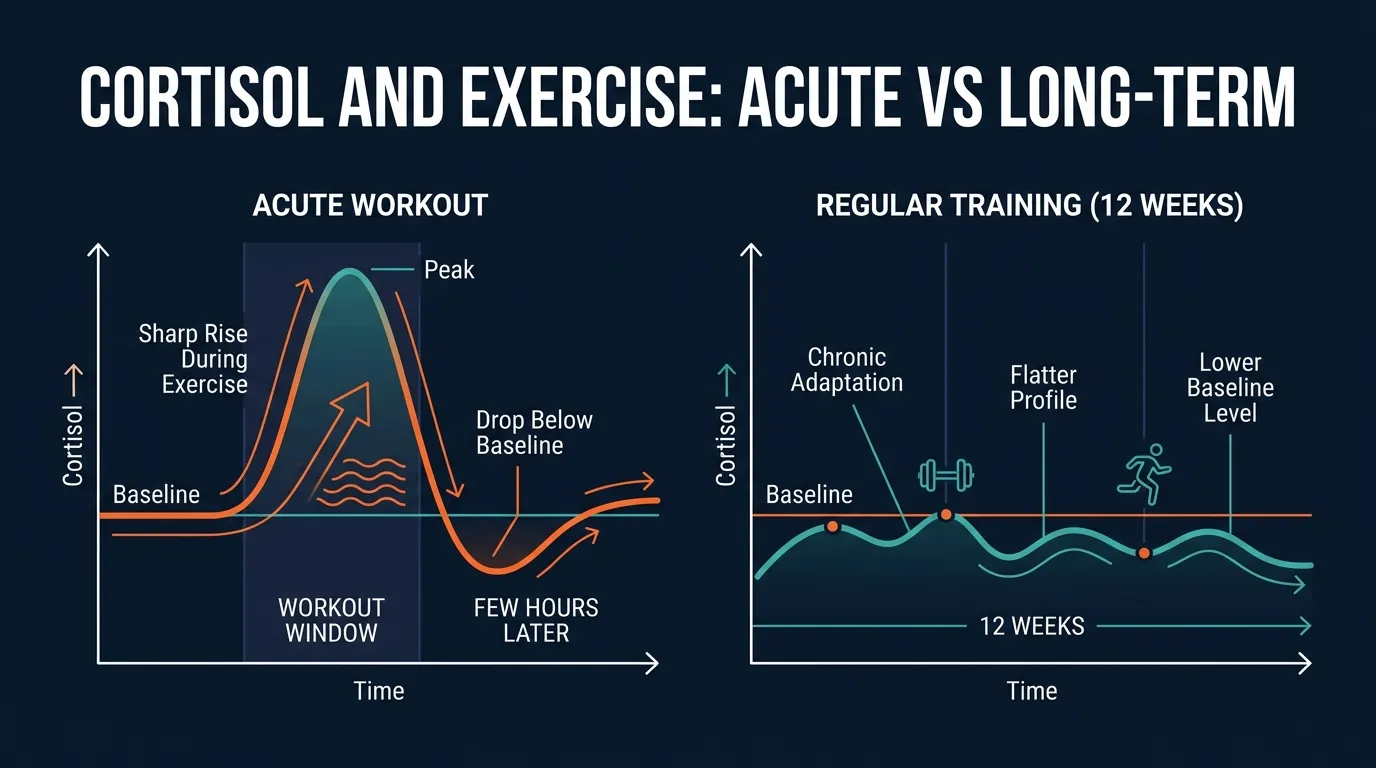
"Is exercise raising my cortisol?" became one of the most-searched fitness questions of 2026. TikTok deserves some of the credit. The viral cortisol face trend convinced a lot of people that a stressful job and a sweaty workout were quietly puffing out their cheeks and ruining their sleep. The actual research is more interesting and a lot less dramatic.
Here is the short version. Yes, a hard workout briefly raises cortisol. That is the point. Cortisol is the signal that mobilizes glucose and fat for fuel during exertion. After the session, levels fall, often a bit below where they started. Across weeks of consistent training, the resting baseline tends to drop, and the body becomes less reactive to other stressors. The exception is overtraining, where chronically pushing too hard with too little recovery flattens the whole cortisol curve.
This article walks through what cortisol actually is, what acute and chronic exercise do to it, the verdict on cortisol face, the overtraining trap, and how to use this information to train smarter without falling into the panic spiral that the algorithm wants you in.
What Cortisol Actually Does
Cortisol gets demonized online, which is unfortunate because you would not be alive without it. It is a glucocorticoid hormone made in the adrenal cortex, regulated by the hypothalamic-pituitary-adrenal (HPA) axis, and it does several jobs your body can't skip.
Cortisol's Day Job
- Mobilizes glucose from the liver so muscles and brain have fuel
- Supports blood pressure regulation
- Modulates immune and inflammatory responses
- Helps you wake up. Cortisol naturally peaks 30 to 45 minutes after waking, the so-called cortisol awakening response
Levels follow a clear daily rhythm. High in the morning, lower across the day, lowest in the early part of the night. That diurnal pattern is healthy and well-regulated cortisol behavior. The problem is not cortisol itself. It is when the rhythm flattens, the peaks blunt, or the system stays activated when it should be settling down.
Why Exercise Triggers a Cortisol Response
Exercise is a controlled physical stress. Your nervous system reads the rising heart rate, lactate, and energy demand and asks the HPA axis for support. Cortisol joins adrenaline in lifting blood glucose and breaking down fat for fuel. Athanasiou and colleagues (2023) reviewed how the stress system responds to different exercise types in Reviews in Endocrine and Metabolic Disorders, and the picture is consistent. Brief, hard work activates the HPA axis. Easy or short work barely budges it. Long, moderate aerobic work raises cortisol slowly and predictably, then lets it fall.
None of that is dangerous in a healthy person. It is the system doing exactly what it evolved to do.
What a Single Workout Does to Cortisol
The acute story has been studied for decades. The cleanest finding is an intensity threshold.
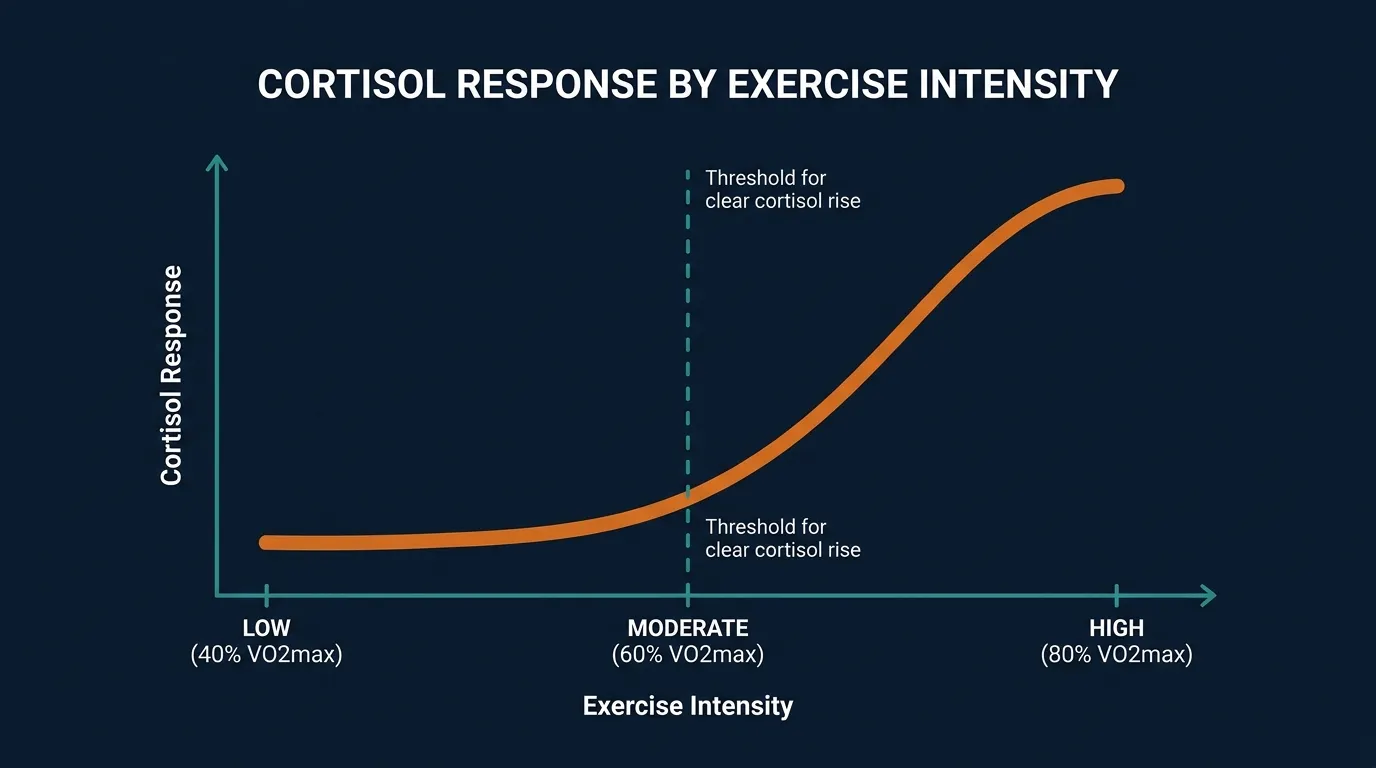
The 60 Percent VO2max Threshold
A landmark study by Hill and colleagues (2008) in the Journal of Endocrinological Investigation tested healthy men exercising at 40, 60, and 80 percent of their maximal oxygen uptake. At 40 percent (an easy walk for most people), cortisol actually trended slightly downward during the session. At 60 percent, cortisol rose modestly. At 80 percent, the spike was steep and significant.
That gives you a rough mental model. Below the heavy-breathing zone, exercise is essentially neutral or calming for cortisol. Above it, expect a transient spike. The spike is the point. It mobilizes the fuel you need to keep working.
How Long the Spike Lasts
For most people, peak cortisol shows up in the bloodstream during or right after the session, then returns toward baseline within 60 to 120 minutes. Salivary cortisol often dips slightly below baseline 2 to 3 hours later. By 24 hours, cortisol is back where it started or modestly lower if the session was tough enough to leave you tired the next day.
Resistance training behaves similarly. Heavy compound work with short rest intervals provokes the largest spike. Light, technique-focused work with long rests produces almost no rise. The hormonal response tracks the metabolic stress of the session, not the moral weight you assign to it.
What Regular Training Does to Cortisol
Acute and chronic effects are different stories, and that is where most TikTok takes go wrong. Just because a single sprint workout spikes cortisol does not mean a sprint program raises your average cortisol over time. The opposite tends to be true.
The 2025 Network Meta-Analysis
The clearest synthesis on this question came out last year. Bartholomew and colleagues (2025) published a network meta-analysis in Sports covering 3,284 adults with psychological distress across studies dated 2003 to 2025. They compared yoga, continuous aerobic exercise, resistance training, multicomponent training, and HIIT against control conditions for cortisol reduction.
The headline finding: every modality except HIIT reduced cortisol relative to control. Yoga showed the largest average reduction. Continuous aerobic exercise was second. Multicomponent and resistance training also helped, but with smaller effects. Most effective programs ran roughly 12 weeks, with three sessions per week of about 55 minutes per session.
HIIT being the odd one out is interesting but not damning. Short, very hard sessions provoke the biggest acute spikes, and in stressed populations they may not produce the calming downstream effect that steady aerobic work does. For people who feel wired, fried, or anxious, the meta-analysis nudges you toward yoga or moderate cardio rather than 30 minutes of all-out intervals.
The De Nys Meta-Analysis
Earlier work pointed in the same direction. De Nys and colleagues (2022) in Psychoneuroendocrinology ran a meta-analysis on physical activity, cortisol, and sleep. They found a small but reliable improvement in diurnal cortisol slope (the steepness of the morning-to-night drop) in people who were physically active. Steeper slopes are healthier. Flat slopes are associated with chronic stress, depression, and metabolic dysfunction.
So consistent training appears to nudge cortisol back into a healthy daily rhythm, especially in people whose rhythm is already off.
What This Means for Stress Reactivity
Trained people don't just have lower resting cortisol on some measures. They also tend to react less to non-exercise stressors. A heated meeting, a near-miss in traffic, or a difficult email produces a smaller cortisol spike in someone who exercises regularly. That dampened reactivity is one of the underrated mental-health benefits of staying consistent. Our explainer on dopamine and exercise covers a parallel adaptation in the reward system, and the exercise and depression research summary walks through the antidepressant effects.
Ready to put this into practice?
Take the free FitCraft assessment and get a personalized plan built on behavioral science, not willpower.
Take the Free Assessment Free · 2 minutes · No credit cardThe Cortisol Face Myth
"Cortisol face" took off on TikTok in 2024 and 2025. The pitch: stress raises cortisol, cortisol puffs your cheeks, your face looks rounder, and the cure is supplements, breathwork, and walking more. Some of that is fine advice for unrelated reasons. The cortisol mechanism is mostly wrong.
What Dermatologists Say
True cortisol-driven facial puffiness, often called moon face, is a clinical sign. It shows up in Cushing's syndrome, a rare endocrine condition usually caused by a tumor or by long-term high-dose steroid medication. Dermatologists who have weighed in on the trend have pointed out that no published research shows everyday psychological stress producing enough cortisol to round out a healthy person's face. Healthline's coverage of the trend includes interviews with dermatologists making exactly this point.
Most face puffiness is something far less exotic. Poor sleep. Alcohol. Salty dinner. Allergies. A late-night cry. Being slightly dehydrated. Your face moves around. That is normal.
Why the Trend Stuck Anyway
Wellness content thrives on monocausal stories. One villain (cortisol). One cure (supplements, breathing, a low-impact workout). The cortisol-face story stuck because it gave people a name for a vague feeling of looking off, and a clean checklist of fixes. The fixes themselves are mostly fine. The mechanism is overstated.
If your face looks puffy, sleep more, drink water, ease off salt and alcohol for a week, and see what happens. If it persists or comes with weight gain, easy bruising, or muscle weakness, see a doctor. Don't diagnose Cushing's from a phone camera.
The Real Risk: Overtraining and a Flattened Cortisol Curve
The version of cortisol-and-exercise that does deserve attention is overtraining syndrome (OTS). This is not "I am tired after leg day." It is months of high training load with insufficient recovery, and it produces a measurable disturbance in the HPA axis.
What the EROS Study Found
The Endocrine and Metabolic Responses on Overtraining Syndrome study, published as Cadegiani and Kater (2017) in Sports Medicine - Open, compared overtrained athletes to healthy trained athletes and sedentary controls. Counterintuitively, the overtrained athletes did not show sky-high resting cortisol. They showed a blunted cortisol awakening response, lower morning peaks, and reduced cortisol response to exercise stimulation tests. The dysfunction sat in the hypothalamus and pituitary, not the adrenals.
That matters because the popular story (push too hard, cortisol stays high, you stay wrecked) is exactly backwards. The body's adaptive response to chronic overload is to dampen the system, not amplify it. A flattened cortisol curve correlates with the fatigue, mood disturbance, and performance decline that define OTS. Our deeper writeup on overtraining syndrome research covers the symptoms and recovery protocol.
Signs You're Drifting Toward Overtraining
- Workouts that used to feel hard now feel pointless or slow
- Resting heart rate creeping up over weeks
- Sleep getting worse despite training more
- Persistent mood drop, irritability, or low motivation
- Strength or endurance going backward
- Frequent minor illnesses
The fix is dull and effective. More sleep. More food, especially carbs. Two to four weeks at half your usual training volume. No new high-intensity blocks until energy and mood normalize. Pushing through is what extends the problem.
How to Train So Cortisol Works for You
Knowing all of this, here is the practical version. None of it is exotic.
Make Most of Your Training Moderate
The classic 80/20 split holds up well in the cortisol literature. Roughly 80 percent of your weekly training should sit at conversational, easy-to-moderate intensity. The remaining 20 percent can include harder intervals, lifting, or sport-specific high-intensity work. That mix gives you the adaptive benefits of the hard sessions without sustained HPA axis activation.
Match Your Hard Days to Your Sleep
Cortisol regulation rides on sleep more than on any supplement. If you slept badly, downgrade today's session. A high-intensity workout on top of a 5-hour night doubles down on the stress signal. A moderate walk or yoga session on those days actually pulls cortisol back toward baseline. Our piece on working out when tired covers the calls to make in real time.
Add Yoga or Mobility Once a Week
The 2025 meta-analysis found yoga produced the largest cortisol reductions in distressed populations. You don't need to convert your entire program. One 30 to 45 minute session per week is enough to deliver the parasympathetic nudge. The yoga and mobility at home guide has a starting routine that needs zero equipment.
Don't Time-Manipulate Cortisol
You will see content telling you to never lift in the morning because of the cortisol awakening response. Skip it. The morning rise is normal and healthy. Exercising on top of it does not produce harm in healthy people. Train at the time of day you can actually keep showing up. Consistency beats biohacking by a wide margin.

Why Most People Spike Cortisol Without Meaning To
Plenty of well-intentioned routines accidentally crank the stress signal. The most common pattern looks like this. Someone gets motivated, signs up for an app or a class, and starts doing five high-intensity workouts a week on too little food and too little sleep. Two weeks in, they feel wrecked. They blame their willpower and quit. The cortisol curve never even got a chance to adapt.
This is the inconsistency loop in a different costume. The underlying problem is not that exercise is bad for cortisol. It is that programs built for an idealized version of you (perfectly rested, well-fed, never sick) collapse on contact with the real you. We covered the broader pattern in the willpower myth, and the fix is the same: programs should adapt to the human, not the other way around.
That is why FitCraft programs reduce volume on days you slept poorly, swap a hard session for mobility when you are stressed, and progress slowly enough that your nervous system gets to keep up. Ty, the 3D AI coach, demonstrates each move, schedules the next session, and adjusts in real time when life gets in the way. Cortisol responds well to that kind of patient, consistent stimulus. It does not respond well to hero workouts followed by two weeks off.
What This Means for You
If you have been worried that your workout is "wrecking your cortisol," the research mostly says relax. A hard session briefly raises cortisol. A regular training habit lowers your average and softens your reactivity to ordinary stress. Yoga and steady aerobic work do this best. HIIT in moderation is fine. HIIT every day, on top of poor sleep and skipped meals, is the version that backfires.
If your face looks puffy, look at sleep, salt, alcohol, and allergies before blaming cortisol. If you feel chronically wrung out, pull back training for two to four weeks and see if energy returns. And if you keep starting and stopping, stop assuming the problem is willpower. The evidence points elsewhere.
Train moderately. Train consistently. Respect rest. Cortisol will sort itself out.
Frequently Asked Questions
Does exercise raise or lower cortisol?
Both, depending on the time scale. A single hard workout briefly raises cortisol, with the spike showing up clearly above about 60 percent of VO2max. Across weeks of regular moderate training, baseline cortisol and stress reactivity tend to fall. Yoga and continuous aerobic exercise produce the largest reductions in people with psychological distress, while HIIT shows the smallest effect.
Is cortisol face real?
For most people, no. The TikTok cortisol face trend blames everyday stress for puffiness, but dermatologists say garden-variety stress does not produce enough cortisol to round out a face. True cortisol-driven facial swelling, called moon face, is a sign of Cushing's syndrome or long-term steroid use, not a busy work week. Most facial puffiness is poor sleep, alcohol, salty food, or allergies.
What kind of exercise lowers cortisol the most?
A 2025 network meta-analysis of 3,284 adults with psychological distress found yoga produced the largest cortisol reductions, followed by continuous aerobic exercise. Most effective programs ran around 12 weeks, three sessions per week, about 55 minutes per session. HIIT was the only modality that did not significantly reduce cortisol in this analysis.
Can too much exercise raise cortisol long-term?
Acutely yes, chronically the picture flips. Athletes with overtraining syndrome often show a blunted morning cortisol response, not a permanently high one. Research from the EROS study suggests the hypothalamus and pituitary, not the adrenals, become less responsive after months of excess training and inadequate recovery. The fix is more rest, fewer high-intensity sessions, and better sleep, not pushing harder.
Does morning exercise spike cortisol in a bad way?
No. Cortisol naturally peaks within an hour of waking, and exercising on top of that morning spike does not appear to cause harm in healthy people. Evening levels typically drop low again as part of the normal diurnal rhythm. Pick the time of day you can actually stick to.